Where is pelvic pain located & how does it feel?

Pelvic pain occurs both in men and women but is more common among women indicating that there might be an issue with the reproductive organs and can stem from other causes. This article explores what is pelvic pain, why pelvic pain occurs, and pelvic pain treatments, among other things. The cause of pelvic pain varies with no evident disease and fluctuating intensity. This pain might be a symptom of an infection in the uterus, ovaries, fallopian tubes, cervix, or vagina. It is considered acute if the pain is sudden, severe, or chronic and keeps coming and going for months. If the pain lasts longer than 6 months with no signs of improvement, it is considered chronic pelvic pain. This pain usually occurs every month, in coordination with menstruation when the egg is released and might be accompanied by fever, nausea, vomiting, sweating, or lightheadedness. Depending on the cause, medications like pain relievers, hormone treatments, or antibiotics coupled with physical therapy, spinal cord stimulation, and trigger point injections can be used to treat the pain.
Pelvic pain during pregnancy is termed pregnancy-related pelvic girdle pain (PGP) or symphysis pubis dysfunction (SPD), which can be treated by: physiotherapy (to keep the pelvis and hip joints moving normally), exercise (to strengthen the pelvic floor, back, and hip muscles), resting in water (buoyancy helps to reduce the pressure on joints), equipment like pelvic support belts, maternity bands and compression pantyhose (it lifts the belly and gives it support) and various prenatal massages, pregnancy pillows are a few ways on how to reduce pelvic pain during pregnancy.
Table of Contents
Feel free to skip ahead if one topic catches your eye:
- Where is pelvic pain located?
- Common reasons for pelvic pain in women
- How are causes of pelvic pain diagnosed?
- When to see a Gynecologist?
1. Where is pelvic pain located?
Pelvic pain usually originates from the genital, internal organs, which spread to muscles and connective tissue (ligaments) and cause pain in the structures of the pelvic floor. This region may also feel tender when touched. The round ligament that stretches it gives a sharp, stabbing pain in the abdomen. This ligament is present from the top of the uterus and ends in the groin. Pelvic pain stretches from the lower back to the perineum to the thighs. Pelvic pain is usually sharp and cramping with pressure or heaviness deep from the pelvis. It may cause pain during intercourse, during a bowel movement or urinating, and even while sitting for long hours. This discomfort may intensify after standing for long periods and can be relieved while lying down. The pain might be mild but still annoying, or even sometimes so severe that one must miss work, can't sleep, and can't exercise.
2. Common reasons for pelvic pain in females
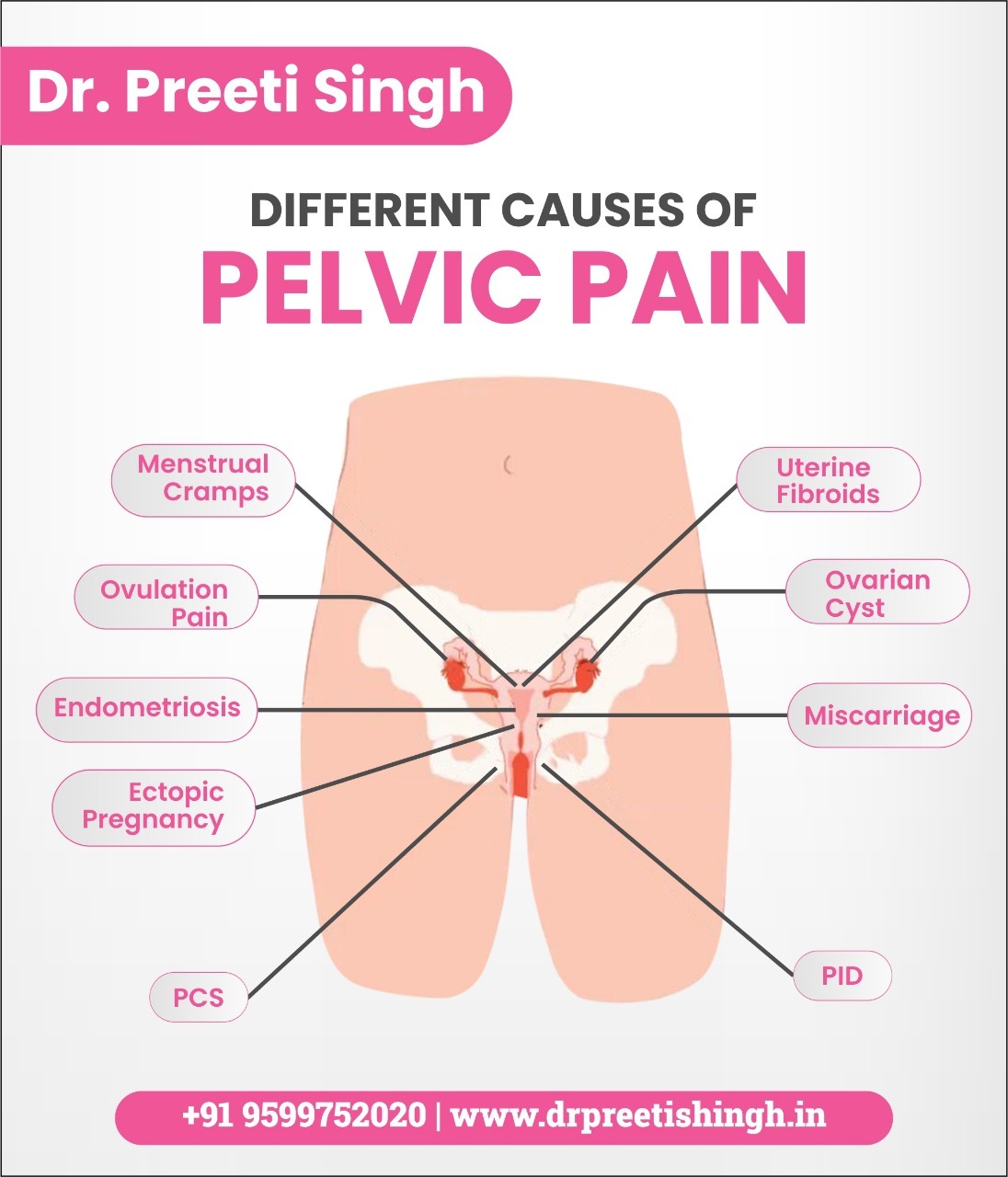
The cause of female pelvic pain varies with no evident disease and fluctuating intensity. Pelvic pain can be due to a gynaecological symptom. Sometimes, pelvic pain indicates an infection or issue with the reproductive system or other organs. Pelvic pain also signifies menstrual cramps, ovulation, or gastrointestinal issues such as food intolerance. Pelvic can also occur due to more serious problems such as interstitial cystitis, urinary tract or sexually transmitted infections, pelvic inflammatory disease, endometriosis, irritable bowel syndrome, appendicitis, urinary stones, ectopic pregnancy or pelvic adhesions, ovarian cysts, uterine fibroids or tumours.
Endometriosis: In this condition, the uterine lining grows outside your uterus. This does not allow the blood and tissue to exit your body through your vagina. They remain in your abdomen, where they may lead to the formation of painful cysts or fibrous band adhesions
Musculoskeletal problems: Inflammation in the pubic joint (pubic symphysis) or hernia can lead to recurring pain in pelvic region.
Chronic pelvic inflammatory disease: This condition occurs due to a long-term infection, usually sexually transmitted involving the pelvic organs.
Fibroids: These are noncancerous growths in the uterus, which may cause a feeling of heaviness in the lower abdomen.
Irritable bowel syndrome: Along with irritable bowel syndrome bloating, constipation or diarrhoea can lead to pelvic pain and pressure.
Painful bladder syndrome: Also known as interstitial cystitis, causes recurring pain in the bladder and a frequent need to urinate. Pelvic pain may arise as the bladder fills, which may improve temporarily after urinating.
Pelvic congestion syndrome: Varicose-type veins around the uterus and ovaries also results in pelvic pain.
Psychological factors: Depression, chronic stress, and sexual or physical abuse may also increase the risk of chronic pelvic pain. Distress makes the pain worse, and chronic pain contributes to emotional distress forming a vicious cycle.
3. How are causes of pelvic pain diagnosed?
To diagnose the cause of pelvic pain, the patient's complete medical history and symptoms need to be monitored closely. A physical exam, along with other tests, helps in diagnosing the cause. The specific testing performed depends on the discussions with the concerned doctor on examination. Some diagnostic tools used are:
- Blood and urine tests.
- Pregnancy tests in females of reproductive age.
- Vaginal or penile cultures to check for sexually transmitted diseases (STD).
- Abdominal and pelvic X-rays to check for organ abnormalities or growths.
- Diagnostic laparoscopy to have a direct look at the structures in the pelvis and abdomen.
- Hysteroscopy to examine the uterus.
- Stool guaiac test to check the stool sample for the presence of microscopic blood.
- Lower endoscopy or colonoscopy, or sigmoidoscopy to examine the inside of the rectum and part or all the colons.
- Ultrasound to provide images of internal organs.
- CT scan of the abdomen and pelvis produces cross-sectional images of the body.
4. When to see a Gynecologist?
In general, with any chronic pain, it is difficult to know when to visit a doctor. It is advisable to visit the doctor if pelvic pain worsens while doing daily chores and the pain is constant, steadily worsening, along with the below-mentioned warning signs. In women with pelvic pain, these symptoms are considered warning signs and need concern:
- Lightheadedness and sudden loss of consciousness with episodes of fainting, syncope, or blood pressure dropping to dangerously low levels.
- Vaginal bleeding occurs even after menopause, along with pelvic pain.
- Fever or chills, or headaches accompanied by spotting.
- Burning sensation while urinating and frequent urination along with pelvic pain.
- Very painful menstrual cramps with recurring or chronic pelvic pain along with the heavy flow.
- Sudden and severe pain, accompanied by nausea, vomiting, excessive sweating, or sometimes agitation.
For more information visit:https://drpreetisingh.in/